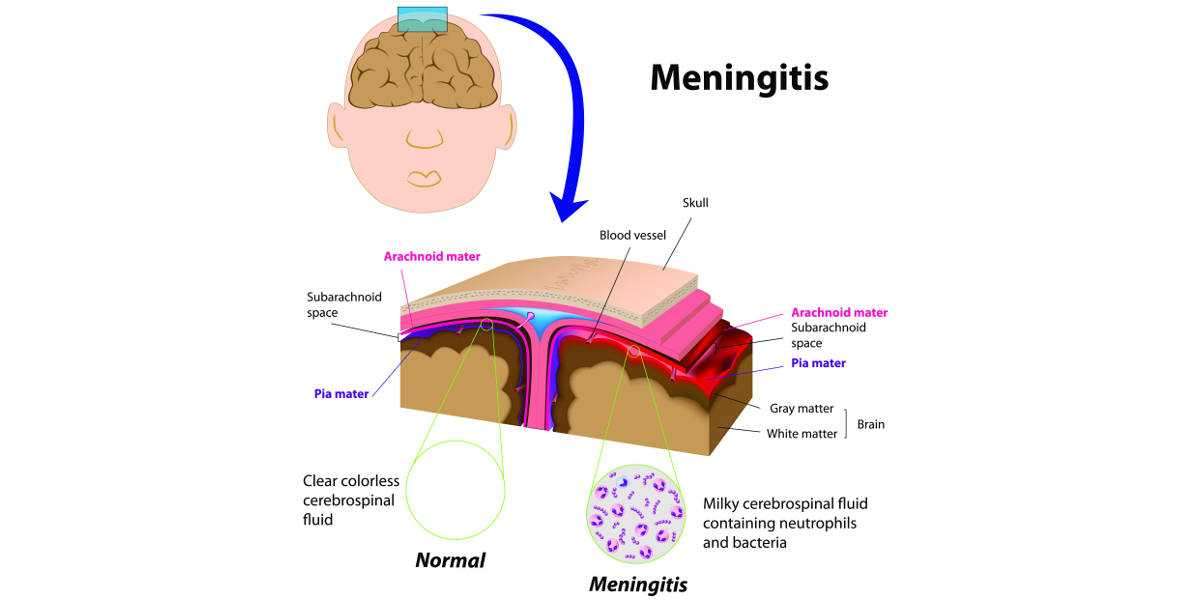
Meningitis is an acute inflammatory condition of the meninges the protective membranes covering the brain and spinal cord. It can be caused by bacteria, viruses, fungi, or, less commonly, parasites and non-infectious conditions. Among these, bacterial meningitis is the most severe and is often associated with significant long-term complications. Despite advances in antimicrobial therapy, including broad-spectrum agents such as ceftriaxone, survivors may experience lasting neurological and systemic effects.
Understanding Meningitis and Its Causes
Meningitis occurs when infectious pathogens invade the cerebrospinal fluid (CSF) and meninges, triggering inflammation. The most common bacterial causes include:
Neisseria meningitidis
Streptococcus pneumoniae
Haemophilus influenzae
Viral meningitis is often caused by enteroviruses, while fungal meningitis may occur in immunocompromised individuals.
Bacterial meningitis is a medical emergency. Immediate empirical antibiotic therapy is critical, and third-generation cephalosporins such as ceftriaxone are frequently used due to their excellent central nervous system penetration and broad antimicrobial coverage. Ensuring access to a certified ceftriaxone injection supplier is essential in both hospital and public health settings to reduce morbidity and mortality.
Why Long-Term Effects Occur
The long-term effects of meningitis are largely due to:
Inflammatory damage to neural tissue
Increased intracranial pressure
Vascular compromise and cerebral infarction
Direct bacterial toxin-mediated injury
Even when antimicrobial therapy eradicates the infection, residual structural and functional damage to the brain and auditory pathways can persist.
1. Cognitive Impairment
One of the most common long-term consequences of meningitis is cognitive dysfunction. Survivors may experience:
Memory loss
Reduced attention span
Impaired executive functioning
Learning difficulties
Children are particularly vulnerable because their brains are still developing. Pediatric survivors may show delayed speech acquisition, poor academic performance, or behavioral changes.
Adults may struggle with concentration, processing speed, and short-term memory deficits. These impairments are often subtle but can significantly impact quality of life and occupational functioning.
2. Hearing Loss
Sensorineural hearing loss is one of the most well-documented sequelae of bacterial meningitis. Inflammation can damage the cochlea or auditory nerve, leading to partial or complete hearing impairment.
Hearing loss may:
Develop during the acute phase
Appear weeks after recovery
Be unilateral or bilateral
The risk is particularly high with infections caused by Streptococcus pneumoniae. Early diagnosis and prompt treatment with appropriate antibiotics from a reliable ceftriaxone injection supplier may reduce the incidence of auditory complications, though not eliminate it entirely.
Children with post-meningitis hearing loss often require cochlear implants, hearing aids, and speech therapy.
3. Seizure Disorders and Epilepsy
Post-meningitic epilepsy is another significant long-term effect. The inflammation associated with meningitis can lead to cortical scarring, gliosis, or structural brain injury, all of which increase seizure risk.
Risk factors include:
Prolonged seizures during acute illness
Delayed antibiotic administration
Cerebral infarction
Subdural effusions
Some patients develop chronic epilepsy requiring lifelong antiepileptic therapy. The likelihood of seizure disorders increases with the severity of the initial infection.
4. Motor Deficits and Paralysis
Damage to motor pathways in the brain can result in:
Hemiparesis (weakness on one side of the body)
Coordination problems
Spasticity
Fine motor impairment
In severe cases, cerebral infarction secondary to vasculitis may occur, leading to stroke-like symptoms. These deficits can persist long after infection resolution and may require long-term physical therapy and rehabilitation.
5. Behavioral and Psychological Changes
Survivors of meningitis sometimes exhibit significant psychological or behavioral changes, including:
Mood disorders (depression, anxiety)
Irritability
Personality changes
Social withdrawal
Children may develop attention-deficit symptoms or conduct issues. Adults may experience post-traumatic stress related to hospitalization or critical illness.
The neuroinflammatory process can alter neurotransmitter systems, while the emotional stress of severe illness contributes to psychiatric outcomes.
6. Hydrocephalus
Meningitis can obstruct cerebrospinal fluid pathways, leading to hydrocephalus an abnormal accumulation of fluid within the brain’s ventricles. This condition increases intracranial pressure and may require surgical intervention, such as ventriculoperitoneal shunt placement.
Untreated hydrocephalus can cause progressive cognitive decline, motor dysfunction, and visual disturbances.
7. Vision Problems
Optic nerve inflammation or increased intracranial pressure may result in:
Blurred vision
Double vision
Visual field defects
Permanent vision loss
While less common than hearing loss, visual complications significantly affect quality of life and may require ongoing ophthalmologic care.
8. Chronic Headaches
Persistent headaches are frequently reported after recovery. These may resemble migraines or tension-type headaches and can continue for months or years.
The exact mechanism is not fully understood but may involve:
Residual inflammation
Altered pain processing pathways
Psychological stress
9. Endocrine Dysfunction
In rare cases, inflammation can affect the hypothalamic-pituitary axis, leading to hormonal imbalances. This may manifest as:
Growth delays in children
Thyroid dysfunction
Adrenal insufficiency
Puberty disturbances
These complications are uncommon but highlight the systemic impact meningitis can have.
Risk Factors for Long Term Complications
Several factors increase the likelihood of persistent effects:
Delayed treatment
Severe bacterial infection
Age (infants and elderly at higher risk)
Immunocompromised status
Infection caused by highly virulent organisms like Neisseria meningitidis
Rapid administration of effective antibiotics often including ceftriaxone plays a crucial role in reducing complications. Hospitals must ensure consistent procurement from a certified ceftriaxone injection supplier to maintain treatment readiness, especially in high-incidence regions.
Prevention and Mitigation
Vaccination
Vaccines significantly reduce meningitis incidence. Immunization programs targeting Haemophilus influenzae and pneumococcal and meningococcal strains have lowered global disease burden.
Early Diagnosis and Treatment
Empirical intravenous antibiotic therapy should begin immediately upon clinical suspicion. Delays increase the risk of neurological injury. Pharmaceutical supply chain integrity including partnership with a reputable ceftriaxone injection supplier ensures timely drug availability.
Adjunctive Therapies
Corticosteroids such as dexamethasone may reduce inflammatory damage and lower the risk of hearing loss in certain types of bacterial meningitis.
Rehabilitation
Long-term management may include:
Speech therapy
Physical therapy
Occupational therapy
Psychological counseling
Audiological support
Early intervention improves outcomes significantly.
Conclusion
The long-term effects of meningitis can be profound and life-altering. Survivors may experience cognitive impairment, hearing loss, seizure disorders, motor deficits, psychological changes, hydrocephalus, and other neurological complications. The severity of these outcomes depends on the causative organism, patient age, immune status, and critically the speed and effectiveness of treatment.
Timely administration of appropriate antibiotics such as ceftriaxone is central to reducing morbidity. Healthcare systems must prioritize early diagnosis, vaccination strategies, and dependable pharmaceutical sourcing, including collaboration with a certified ceftriaxone injection supplier, to optimize patient outcomes.
While many individuals recover fully, ongoing monitoring and multidisciplinary rehabilitation are essential for those facing persistent complications. Through prevention, prompt treatment, and structured follow-up care, the long-term burden of meningitis can be substantially reduced.